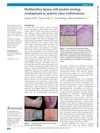
Systemic Lupus Erythematosus in India: A Clinico-Serological Correlation
June 2022
in “
Cureus
”

TLDR Early identification of lupus through skin signs and blood tests is crucial in India.
The study on systemic lupus erythematosus (SLE) in India, involving 40 patients, found that the mean age of onset was 23.3 years with a female to male ratio of 19:1. Common skin lesions included malar rash (77.5%), photosensitivity (70%), and non-scarring alopecia (60%). Systemic manifestations frequently observed were arthritis (77.5%) and nephritis (30%). Among patients with only cutaneous manifestations, a significant number had positive serological markers such as antinuclear antibody (85%) and anti-double-stranded DNA (57%). The findings suggest that early identification of SLE through skin lesions and serological profiles can precede systemic symptoms, highlighting the importance of environmental factors in the Indian context.